Devyser launches the first IVDR compliant NGS assay for thalassemia and sickle cell disease testing
Devyser, today announced the launch of Devyser Thalassemia v2, the first Next-Generation Sequencing...
Post-transplantation
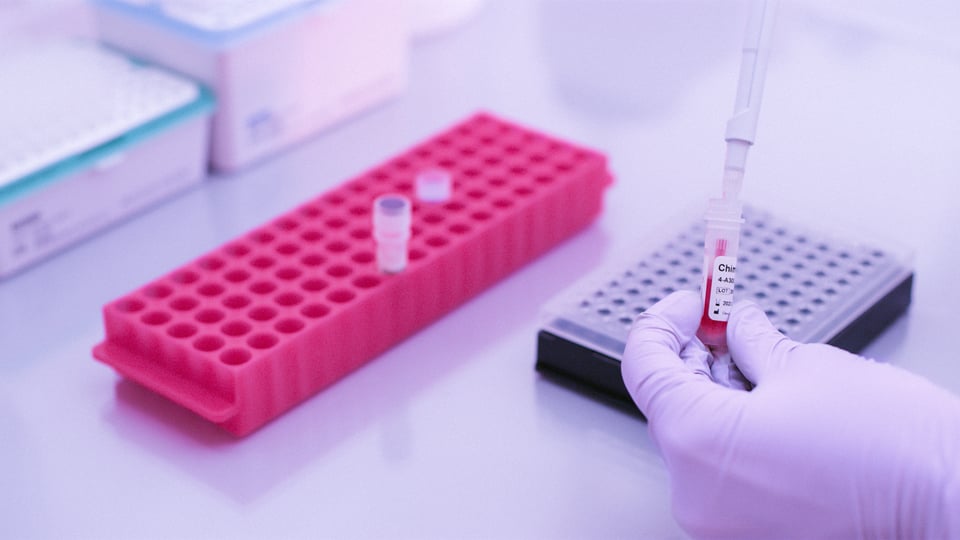
Post-transplantation | October 7, 2022
Chimerism monitoring after hematopoietic stem cell transplantation (HSCT) plays a key role in assessing engraftment status and predicting serious complications to allow timely and effective therapeutic intervention. For optimal clinical utility, assays for chimerism monitoring need to be highly sensitive, accurate and precise across a wide dynamic range.
Here’s why today’s most widely used chimerism assays fall short of the ideal, and why the latest high-sensitivity technology has the potential to set a new ‘gold standard’ for chimerism assessment.
Over the past 60 years, significant strides have been made in HSCT. Early human bone marrow transplants were fraught with failure and limited to only the most life-threatening cases. Today, HSCT has become the prevailing curative treatment for many non-malignant and malignant diseases, with more than 50,000 HSCTs performed annually in over 1,500 transplant centers worldwide.
Alongside the evolution of HSCT, the advancement of chimerism monitoring has played a central role in enabling clinicians to better evaluate engraftment status and improve clinical decision-making after allogenic HSCT. The relative amounts of healthy donor and residual recipient cells, and their dynamics over time, provide important clues to whether the patient is at risk of an adverse event such as engraftment, graft-versus-host disease, rejection, or disease relapse. Unlike disease-specific evaluations, chimerism assays are widely applicable even when appropriate markers for minimal residual disease are unavailable.
The adoption of molecular genotyping methods for chimerism assessment has made it easier and faster to reliably identify recipient and donor genotypes and determine their relative fractions in blood, bone marrow or other tissues. Using molecular methods, chimerism status can be assigned to one of several categories:
PCR-mediated analysis of short tandem DNA repeats (STR-PCR) is currently considered the gold-standard method for routine chimerism monitoring. The inherent polymorphism within STR regions makes STR-PCR a very powerful method to discriminate individual genotypes with confidence, provided that an appropriate marker panel is chosen. STR-PCR also has good accuracy and precision at higher levels of mixed chimerism, making it particularly useful when levels of recipient DNA are elevated—for example, in the early stages after transplantation.
Despite these advantages, STR-PCR is only semi-quantitative and lacks the sensitivity needed to reliably detect disease relapse before its clinical manifestation. Lineage-specific analysis has been shown to improve sensitivity as much as 10-fold, but requires additional purification and isolation steps that drive up cost and turnaround times. Drawbacks such as these are driving the development of improved methods for routine monitoring and early detection of relapse.
Relapse is the leading cause of HSCT failure in patients with hematologic malignancies, occurring in 35-45% of cases (https://doi.org/10.1586/ehm.10.32). Patients with MC have a much higher rates of relapse (40-90%) compared to those with complete donor chimerism (10-20%). If MC status is progressive (increasing over time), the prognosis is particularly poor. Moreover, positive correlations have been observed between the rate of chimerism increase and the relative risk of subsequent relapse (https://doi.org/10.1016/j.bbmt.2014.07.003).
Unfortunately, disease treatment after relapse is challenging, with a high risk of failure. Therefore, detecting chimerism early—before it reaches the critical threshold of 1 %, which in certain publications has been shown to be critical for increased risk of relapse —can provide clinicians with more time and more options for effective therapeutic intervention. Donor lymphocyte infusion (DLI), termination of immunosuppression, or re-transplantation with cells of the same or another donor are all options that may improve prognosis if implemented while the malignant cell burden is sufficiently low.
The emergence of quantitative real-time PCR (qPCR) methods for analysis of SNP or indel markers was a significant step forward for sensitivity of MC detection, extending the limit of detection from 1% down to 0.1% or lower, into the range required for quantitative analysis of micro-chimerism.
Evidence to support the diagnostic value of high-sensitivity tests is mounting. For example, a recent longitudinal analysis (https://doi.org/10.1038/s41409-018-0176-7) of 901 samples from 71 patients with hematological malignancies undergoing HSCT found that a high-sensitivity assay based on qPCR was able to exclude relapse with high certainty and predict relapse with high sensitivity and specificity more than a month prior to clinical diagnosis. In more than three quarters of patients who relapsed, chimerism never exceeded 1% prior to clinical diagnosis, and therefore might have been missed by STR-PCR.
Chimerism is typically monitored for at least 5 years post-HSCT. During this time, levels of donor and recipient cells vary widely due to many different and often competing factors, In the early stages post-transplantation, relatively high levels of residual recipient DNA may be present in peripheral blood and bone marrow samples. In the days, months or years following engraftment, very low levels of micro-chimerism may need to be detected against a high background of donor genotype. Accurate quantitative measurement is essential to understand the significance of both subtle and gross changes over time.
The ideal chimerism test should therefore be capable of accurately and reliably detecting chimerism levels regardless of whether autologous cells are present in scarce amounts or at elevated levels. qPCR detection of SNP and indel markers provides high-sensitivity, but not the precision needed to monitor mixed chimerism changes at levels exceeding ~20%. STR-PCR is reliable and precise at higher levels, but not sensitive enough for early detection of relapse.
While parallel use of both STR-PCR and qPCR is one option to cover the full dynamic range, it adds considerable complexity and time to the process. In addition, the need for multiple assay protocols can make data analysis and interpretation more difficult.
One of the most promising technologies for improved chimerism monitoring is next-generation sequencing (NGS). Using novel strategies that combine the benefits of both STR-PCR and qPCR in a single assay, recent research has shown the potential of NGS as an alternative to current methods for high-throughput chimerism monitoring (https://doi.org/10.1016/j.cca.2020.10.034).
In the next article, we’ll take a closer look at how NGS is taking chimerism monitoring to the next level.
For more in-depth information on this topic, read our expert review on overcoming limitations in the detection of mixed chimerism.
.jpg)
Devyser, today announced the launch of Devyser Thalassemia v2, the first Next-Generation Sequencing...
Read More
Devyser Diagnostics AB (publ), a Swedish molecular diagnostics company, today announces that it has...
Read More

Devyser today announced that it entered a strategic agreement with Illumina, a global leader in DNA...
Read More

Devyser is proud to announce that the company has been awarded a tender by Oslo University Hospital...
Read More